
Optimise Your Health Through Perimenopause and Beyond.
Are you in your late 30s, 40s, or 50s and noticing that your body—and life—feel a bit more complicated than before?
You’re not alone.
Hormonal shifts during perimenopause and menopause bring profound changes, yet these stages are rarely discussed openly. Many women struggle silently for years before realizing what’s happening.
During this transition, key hormones like estrogen and progesterone fluctuate dramatically before gradually declining, marking the end of menstrual cycles and fertility.
Some women breeze through it, while others experience challenging symptoms—but one thing is certain: perimenopause is a natural phase of life, not an illness.
Interestingly, humans are one of the few species where females live long past their reproductive years. Research suggests postmenopausal women have historically played a vital role in family and community survival. Families with grandmothers present often had better nutrition and higher child survival rates—testament to their importance.
Yet today, many women juggle careers, family responsibilities, and personal well-being during this hormonal shift, making this a particularly demanding time. Studies show menopause can affect work productivity, career progression, and overall life satisfaction.
The good news? Understanding what’s happening changes everything.
Knowledge gives women the power to advocate for their health, make informed choices, and move through this transition with confidence rather than fear.
So let’s talk about it.
Because when menopause is understood and supported, it can become not just manageable—but empowering.
Understanding Perimenopause and Menopause
Before we go any further, let’s get clear on what perimenopause and menopause actually mean—because these terms are often used interchangeably, and they’re not the same thing.
Perimenopause is the transition phase leading up to menopause. Hormones—especially estrogen and progesterone—fluctuate and gradually decline. Ovulation and menstruation still occur, but periods may become irregular, heavier, or lighter. Symptoms often appear during this stage and it can last several years.
Menopause begins when a woman has gone 12 consecutive months without a period. If periods have stopped due to surgery or medication, menopause can be confirmed through blood tests measuring FSH, LH, and estradiol.
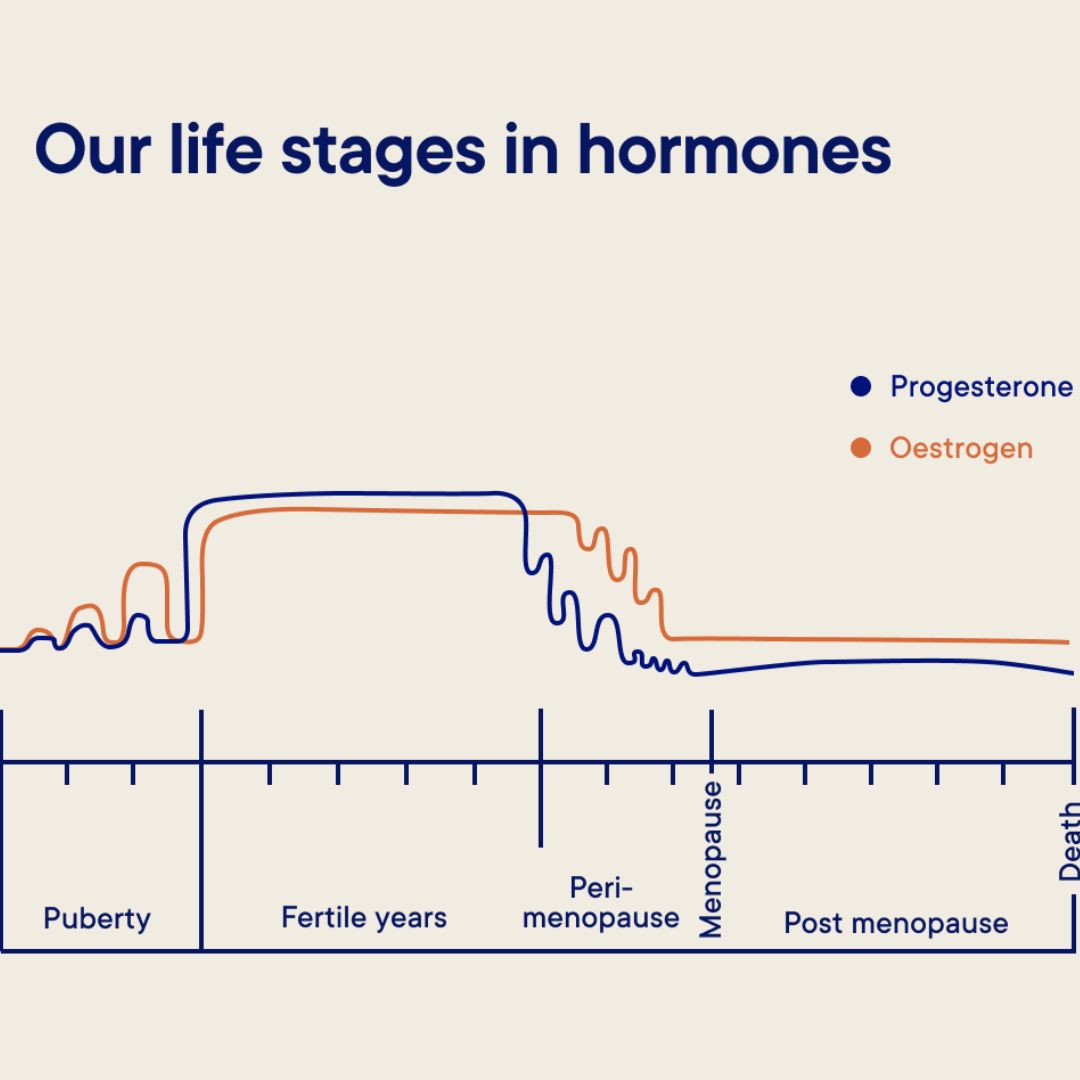
Source: https://www.jennis.com/blog/perimenopause/everything-you-need-to-know-about-perimenopause/
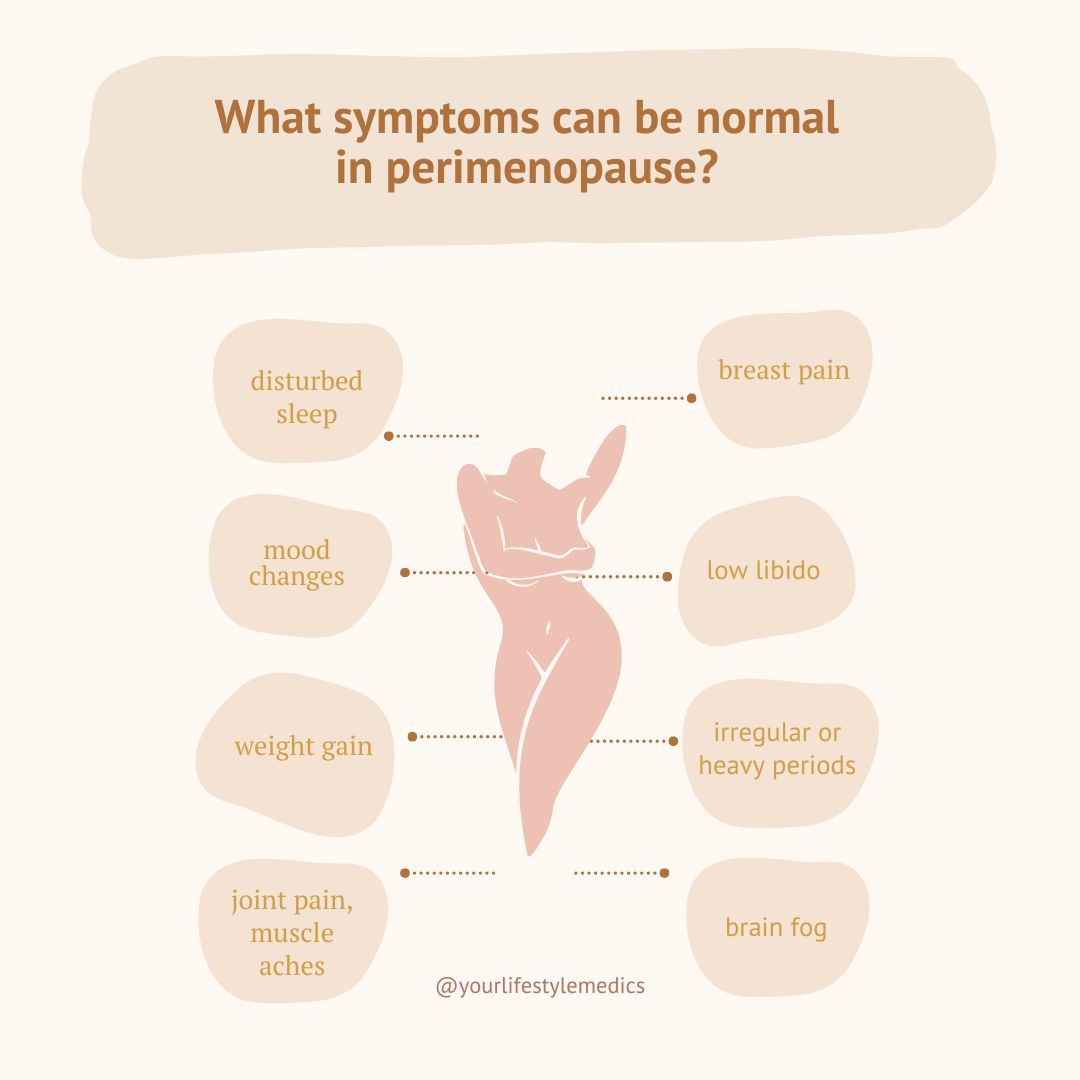
A common misconception is that symptoms only appear after periods stop. In reality, perimenopause can be just as challenging due to unpredictable hormonal swings. Symptoms may include:
- Mood swings, anxiety, depression
- Migraines and heart palpitations
- Joint pain and muscle stiffness
- Brain fog and memory issues
- Poor sleep and chronic fatigue
- Weight gain and metabolic changes
- Hair thinning, dry skin, brittle nails
- Increased cholesterol and blood sugar levels
Why so many symptoms?
Estrogen receptors exist in nearly every cell of the body, so fluctuations can impact brain, heart, and overall health.
Understanding what’s happening beneath the surface is the first step toward managing symptoms and feeling better.
So next, let’s explore how you can start taking back control…and navigate this transition with confidence and well-being.
Phases of Peri/menopause
Very Early Perimenopause (Mid to Late 30s)
In very early perimenopause, your menstrual cycle may remain regular, but subtle changes like worsened PMS, sleep disruption, migraines, or mood changes can appear.
Many women don’t realize these are early signs of hormonal change, and dismiss these shifts as stress or “just getting older,” without realizing they can be the first signs of hormonal change linked to perimenopause.
Early Perimenopause
As perimenopause progresses, progesterone levels typically begin to decline while estrogen remains relatively high. This imbalance happens partly because ovulation becomes less consistent, and progesterone is only produced after ovulation. With less progesterone in the picture, symptoms often become more noticeable.
Supporting progesterone during this phase can make a meaningful difference in symptom management.
You may start to notice:
- Slightly shorter cycles (1–2 days)
- Occasional missed periods (once or twice a year)
- More intense PMS, mood swings, irritability
- Heavier periods
- Anxiety, brain fog, insomnia
- Breast tenderness or pain
- Increased migraines or tension headaches.
These changes often begin gradually, but signal the start of a longer transition that unfolds over several years. Recognizing early perimenopause allows you to take proactive steps to support your hormones, energy, and emotional well-being.
Late Perimenopause and Beyond
In late perimenopause, estrogen levels begin to decline alongside progesterone. Menstrual cycles often become noticeably irregular—periods may be lighter, farther apart, or stop unexpectedly for months at a time.
As estrogen drops, symptoms such as hot flashes, night sweats, and vaginal dryness tend to become more prominent. Once you’ve gone 12 consecutive months without a period, menopause is officially reached. From that point on, you’re considered postmenopausal.

Supporting both estrogen and progesterone through this stage can be key to reducing symptoms and protecting long-term health. Understanding how your body is changing empowers you to make informed choices—and feel your best—through every phase of perimenopause, menopause, and beyond.

The Hidden Impact of Perimenopause and Menopause on Mood and Well-Being
Hormonal shifts strongly influence stress and mood. Lower estrogen can increase cortisol (stress hormone), while reduced progesterone removes its calming effect. This may result in:
- Irritability, anxiety, and “on edge” feelings
- Amplified pre-existing conditions like PMS, ADHD, or depression
Stress can come from multiple sources:
- Psychological: self-criticism, toxic relationships, perfectionism
- Physical: nutrient deficiencies, poor gut health, disrupted sleep
- Environmental: technology overload, excessive artificial light, work or financial pressures
Managing stress:
- Reduce controllable stressors: Set boundaries, delegate, simplify commitments, and get household support.
- Regulate your nervous system: Practice mindfulness, yoga, journaling, nature walks, or gentle exercise.
- Support your body: Eat balanced meals with protein, whole grains, and fiber to stabilize blood sugar and reduce stress effects.
Recognize that this period of life is a time for slowing down and listening to your body, which can have long-term benefits for health and resilience.
Perimenopause doesn’t just affect the body—it can have a profound impact on mood, sleep, and emotional well-being. Sudden mood swings, disrupted sleep, or the onset of anxiety or depression are common during this transition, even in women who’ve never experienced these issues before.
Because these symptoms can look like chronic stress, burnout, mental health conditions, or even pain and fatigue disorders, they’re frequently misdiagnosed. When hormonal changes aren’t considered, many women are left feeling unheard—and without the support they actually need.
While stress and lifestyle factors can contribute, for many women fluctuating hormones are the underlying driver.
Addressing the hormonal shifts themselves—while also taking a holistic approach that supports both body and mind—often leads to far better and more lasting results than simply treating individual symptoms in isolation.
These changes can feel overwhelming, especially when they seem to come out of nowhere. But recognizing the hormonal connection is a powerful first step toward finding clarity, support, and effective solutions. effective relief.
Menopause and Long-Term Health: What You Need to Know
Menopause isn’t just about the end of periods —the drop in estrogen means many of its protective effects disappear, increasing the risk of several long-term health conditions.
These include:
- Heart disease
- Dementia and cognitive decline
- Type 2 diabetes
- High blood pressure
- Osteoporosis (weakened bones)
- Depression and mood disorders
This makes prevention so important during and after menopause, as it’s estimated up to 80% of most chronic health issues can be prevented via lifestyle. Supporting your health through intentional choices isn’t optional—it’s one of the most powerful tools you have to stay strong, resilient, and well in the years ahead.
Interestingly, even after the ovaries stop producing estrogen, the body still makes small amounts through fat tissue. This helps explain why weight gain during menopause is so common—especially around the hips and thighs, where some fat storage is actually normal and protective.
That said, excess weight gain around the abdomen (known as visceral fat) is a different story. This type of fat is metabolically active and inflammatory, meanings it’s linked to a higher risk of metabolic conditions like heart disease and type 2 diabetes.
The encouraging news? There are many effective ways to support your body through menopause and set yourself up for long-term health and vitality.
So let’s explore what you can do to optimize your health, feel your best, and truly thrive during this transition.

A Holistic Approach to Perimenopause and Menopause
Perimenopause and menopause aren’t just about managing symptoms—they represent a significant shift in your body, mind, and overall well-being. A holistic approach recognizes this by supporting the whole person, not just individual complaints.
This includes:
- Regular movement to support metabolism, bone strength, and mood
- Balanced, nourishing nutrition to provide essential nutrients and hormonal support
- High-quality sleep to support recovery, energy, and mental clarity
- Stress management and mindfulness to regulate the nervous system
- Meaningful relationships and social connection to strengthen emotional resilience
While genetics influence when menopause begins and how it unfolds, your health in the years leading up to perimenopause plays a major role in how you experience it. Building strong foundations early can ease symptoms now and reduce the risk of chronic conditions later.
This stage of life is also a critical window for long-term health. Hormonal shifts can reveal underlying imbalances or worsen existing conditions, making a proactive, comprehensive approach essential. That means paying attention to:
- Metabolic health (blood sugar regulation, cholesterol, and heart health)
- Bone health (preventing bone loss and osteoporosis)
- Gut health (nutrient absorption, inflammation, and immune function)
- Nervous system balance (mood, stress resilience, and cognitive health)
- Identifying nutrient deficiencies or other hormonal issues, such as thyroid dysfunction or insulin resistance
By addressing these areas holistically, you can move through perimenopause with confidence—and lay the groundwork for vibrant, empowered health for years to come.

Nutrition Matters: Eating to Support Hormones and Health
What you eat can dramatically influence how you experience perimenopause and menopause. The right diet doesn’t just help reduce symptoms—it can also lower your risk of long-term health issues and support overall vitality. Research shows that a well-balanced eating plan can reduce menopausal symptoms by up to 30%.
One of the most effective approaches? A Mediterranean-style, anti-inflammatory, whole-food, plant-rich diet. This way of eating nourishes your body while supporting:
✓ Heart, brain, and bone health
✓ Hormonal balance and metabolism
✓ Gut health and inflammation control
✓ Immune system function
For example, a 2022 study found that following a Mediterranean diet significantly reduced menopausal and psychological symptoms—especially for individuals with a higher BMI. Key contributors were legumes and extra-virgin olive oil.
Another study linked higher intake of vegetables, whole grains, and minimally processed foods with fewer psychological symptoms, better sleep, and less severe hot flashes, night sweats, and other common menopausal symptoms. Conversely, processed foods, added sugars, saturated fats, and excess caffeine were associated with worse symptoms.
Practical Nutrition Tips To Help You Thrive
What you eat can have a profound impact on how you feel during perimenopause and menopause.
A nutrient-rich, balanced diet can help reduce symptoms, support hormone balance, and protect your long-term health. Here’s how to make your meals work for you:
Smart Food Choices
✓ Choose whole grains over refined carbs – They help maintain steady energy levels, support metabolism, and reduce blood sugar spikes.
✓ Limit ultra-processed foods and added sugars – These increase inflammation and worsen menopausal symptoms.
✓ Swap saturated fats for healthy fats – Use nuts, seeds, avocado, and olive oil instead of fatty meats and full-fat dairy. Keep total fat intake around 30% of daily calories, which may also help reduce hot flashes and night sweats.
✓ Include legumes, seeds, and nuts daily – These provide fiber for gut health and phytoestrogens that gently support hormone balance.
✓ Eat 5+ servings of colorful vegetables daily – Focus on non-starchy, above-ground veggies and include at least two servings of fruit to provide essential vitamins and minerals.
✓ Make leafy greens a daily staple – Packed with calcium, magnesium, vitamin K, B vitamins, and anti-inflammatory compounds, they support bones, mood, and sleep.
✓ Add cruciferous veges wherever you can – Broccoli, kale, cauliflower, Brussels sprouts, and cabbage help with hormone balance, liver detoxification, and overall health protection.
✓ Ensure adequate omega-3 intake – Include fatty fish, flaxseeds, chia, walnuts, and hemp hearts to support heart, brain, and immune function.
✓ Prioritize protein at every meal – Protein balances blood sugar and maintains muscle and bone health. Aim for 1.2–1.6 g/kg/day, increasing after age 65. Most protein should come from plant sources like legumes, nuts, seeds, and whole grains, with moderate inclusion of fish, chicken, or eggs if needed.
✓ Limit red meat to 300g/week, and processed meats to less than 100g/week – This supports heart health and lowers cancer risk.

Key Micronutrients Your Need for Midlife Health
- B12, Iron, Folate & Iodine – Support energy, mental health, and thyroid function.
- Calcium (1200 mg/day) – Essential for bone health; found in tofu, leafy greens, seeds, legumes, and dairy.
- Vitamin K – Supports bones, heart, and brain health; found in dark leafy greens.
- Vitamin D – Crucial for bones, mood, and immunity; aim for sun exposure or supplementation, especially in winter.
Gut Health & Hormonal Balance
Your gut plays a central role in metabolism, inflammation, mood, and hormone regulation. To support it:
✓ Eat at least 30g of fiber daily from a variety of plant foods.
✓ Include probiotic-rich foods like yogurt, kefir, sauerkraut, and kimchi.
✓ Aim for 30 different plant foods per week to nourish a diverse gut microbiome.
Research shows a balanced gut can help reduce menopausal symptoms, improve mood, and support overall health.
The Power of Phytoestrogens
Phytoestrogens are plant compounds that mimic estrogen and gently support hormone balance. They’re found in:
✓ Soy products – tofu, tempeh, edamame, soy milk
✓ Flaxseeds, sesame seeds, chickpeas, whole grains, berries, barley, tea
These compounds act as Selective Estrogen Receptor Modulators (SERMs): they provide estrogen-like effects where needed (reducing menopause symptoms) and block excess estrogen where harmful (supporting breast and uterine health). Studies show soy can improve hot flashes, sleep, cognition, and reduce breast cancer risk—choose whole, minimally processed options.
Time-Restricted Eating (TRE)
Eating within a 10–12 hour window may support weight management, blood sugar stability, and metabolic health. However, extended fasting is not recommended for women with a history of eating disorders or malnutrition.
The Takeaway
Eat to thrive during perimenopause and beyond, by focusing on:
- Whole, plant-rich foods
- A rainbow of colorful vegetables and fruits
- Balanced protein and healthy fats
- Optimizing gut and hormone health
When you nourish your body thoughtfully during this transition, you set yourself up for better energy, mood, and long-term health—your future self will thank you!

Why Limiting Alcohol, Caffeine, and Tobacco Matters
Certain lifestyle factors can have a big impact on how you experience perimenopause and menopause.
Alcohol – While a glass of wine may feel relaxing, alcohol can increase the risk of several cancers (especially breast cancer), disrupt heart and brain health, worsen sleep and mood, and contribute to osteoporosis and hidden weight gain. The general advice is to drink as little as possible, and if you do choose to drink, keep it to no more than 10 units per week.
Caffeine – For most women, caffeine is fine—but it can exacerbate hot flashes and disrupt sleep. If these symptoms are an issue, consider reducing intake or switching to decaf later in the day.
Tobacco – Smoking worsens menopause symptoms (especially hot flashes) and increases risks of heart disease, dementia, and osteoporosis. Quitting—or at least reducing smoking—can dramatically improve your health. Menopause is a great reason to make this change, and there are plenty of support options available through your doctor or quit-smoking programs.

Movement: A Vital Ally in Perimenopause
Maintaining and building muscle mass during perimenopause is essential. As estrogen levels drop, regular movement helps support:
- Metabolic health and body composition
- Blood sugar balance
- Stress reduction
- Circulation to reproductive organs
- Sleep, mood, and energy
- Bone strength
- Even reduction in hot flashes
Getting started:
If you’re new to exercise, any movement is better than none. Aim for 20–30 minutes of moderate-intensity activity daily—enough to raise your heart rate while still allowing conversation. Options include: brisk walking, biking, swimming, pilates, climbing stairs, or even household chores like gardening.
Strength training is crucial:
Perform muscle-strengthening exercises at least 2+ days per week. This can include bodyweight exercises (push-ups, squats, lunges), weightlifting, pilates, yoga focused on strength, or heavy gardening tasks. Strength training preserves muscle mass, which naturally declines with age—women can lose up to 10% of muscle mass during perimenopause. Preserving muscle also supports immune, metabolic, and bone health, helps to improve blood sugar control, and reduces long-term health risks.
To figure out if you are using enough resistance, you should be doing each exercise to the point of fatigue (last 1-2 reps feel very hard), then repeating the sequence 2-3 times.
Some evidence suggests that heavier weights with less reps (ie fatiguing by 5-6 reps) may have added benefits for muscle in peri/menopause – but if you’re just getting started, any exercise helps!
High-intensity exercise:
Some women enjoy HIIT or running, which can boost cardiovascular health, metabolism, and body composition. To avoid overstressing the body, try short HIIT intervals (30s) with 1–2 minutes rest, and skip intense sessions when stressed, unwell, or depleted.
Tips for incorporating movement daily:
- Set small, achievable goals and build them gradually.
- Habit stack exercise with existing routines (e.g., 10 squats while brushing your teeth).
- Move more throughout the day—stand, stretch, or walk for 5 minutes each hour.
- Exercise with a friend or join a class for accountability and motivation.

Sleep: The Foundation of Health
Sleep disruptions are the second most common perimenopause symptom after hot flashes. Hormonal fluctuations, night sweats, stress, and circadian rhythm changes all play a role.
During sleep, your body:
- Repairs tissues
- Removes toxins
- Balances hormones
- Recalibrates the nervous system
Poor sleep can lead to fatigue, irritability, brain fog, metabolic disturbances, lowered immunity, and increased chronic disease risk. Prioritizing sleep is essential for energy, resilience, and overall well-being.
Sleep hygiene tips:
✓Keep a consistent schedule: Go to bed and wake up at the same time every day, including weekends.
✓Create a relaxing bedtime routine: Reading, a warm bath, gentle yoga, or calming music signals your body to wind down.
✓Limit caffeine and alcohol: Avoid caffeine for at least 6-8 hours before bed. Limit alcohol 3–4 hours before sleep, as it can fragment rest. Some women find they sleep far better if they avoid alcohol altogether.
✓Reduce bright light and screens: Use soft lighting at night and limit screens 1–2 hours before bed. Blue-light-blocking apps or glasses can help.
✓Exercise and sunlight exposure: Morning sunlight and regular physical activity regulate your sleep-wake cycle.
✓Natural aids: Herbal teas (chamomile, passionflower), magnesium, or melatonin (where prescribed) may support sleep.
✓HRT: Hormone replacement therapy can be effective for restoring healthy sleep—discuss with your doctor if needed.
For more simple tips check out our sleep article.

Mood and Stress in Perimenopause
Hormonal shifts in perimenopause—especially drops in estrogen and progesterone—can impact stress response and mood regulation. Lower estrogen can increase cortisol (the stress hormone), while reduced progesterone removes its calming effect, leaving many women feeling irritable, anxious, or “on edge.” Pre-existing conditions like PMS, PMDD, ADHD, anxiety, or depression may also intensify.
Sources of stress:
- Psychological: Self-criticism, perfectionism, toxic relationships, multitasking, trauma
- Physical: Skipping meals, too much/little exercise, poor gut health, nutrient deficiencies, disrupted sleep
- Environmental: Excess artificial light, technology overload, negative news, work or financial pressures
Managing stress effectively:
1. Reduce stressors:
- List what causes stress, categorize into controllable vs. uncontrollable.
- Address what you can control: set boundaries, delegate tasks, simplify commitments.
- Practical solutions: meal delivery, cleaners, shared childcare, household support.
2. Regulate your nervous system:
- Mindfulness practices like deep breathing, meditation, yoga, journaling, or spending time in nature calm your body and mind.
- Prioritize time for yourself—refilling your energy is just as important as daily chores and responsibilities.
3. Support your body:
- Eat regularly with whole grains, adequate protein, and fiber to stabilize blood sugar and reduce stress impacts.
- Understand cravings: sugar or refined carbs often spike when stressed but can worsen fatigue and mood.
Recognize that your body and mind are undergoing major natural changes. Slowing down, listening to your body, and practicing self-care during this transition can yield long-term benefits for health and resilience.

Your Peri/menopause Action Plan
1. Understand Your Transition
- Track your menstrual cycle and note changes (cycle length, flow, missed periods).
- Recognize early symptoms: hot flashes, night sweats, mood swings, brain fog, sleep issues, joint pain, weight changes.
- Accept that perimenopause is a natural phase—not a disease – but that addressing symptoms and lifestyle early can make all the difference.
2. Hormone & Health Awareness
- Know your key hormones: estrogen and progesterone.
- Discuss HRT with your doctor if symptoms are severe, or are not improving with lifestyle changes.
- Monitor long-term health markers: blood sugar, cholesterol, waist circumference, bone density, blood pressure.
3. Nutrition
- Eat a Mediterranean-style, plant-rich, anti-inflammatory diet:
- Whole grains, legumes, nuts, seeds
- Colorful vegetables (5+ servings/day) and fruits (2+ servings/day)
- Leafy greens and cruciferous vegetables daily
- Healthy fats (olive oil, avocado, nuts)
- Protein at each meal (1.2–1.6g/kg/day)
- Limit red meat (<300g/week) and ultra-processed foods
- Focus on key micronutrients: B12, iron, folate, iodine, calcium, vitamin D, vitamin K.
- Support gut health: fiber, probiotics, 30 diverse plant foods per week.
- Include phytoestrogens: soy, flax, chickpeas, whole grains.
- Optional: Time-restricted eating (10–12 hour window) if suitable.
4. Movement & Exercise
- Daily moderate activity: 20–30 minutes (walking, swimming, cycling, gardening).
- Strength/resistance training: 2+ times/week (bodyweight exercises, weights, pilates).
- HIIT: Short intervals with rest (30s work, 1–2min recovery) if appropriate.
- Focus on preserving muscle mass to maintain metabolism, bone health, and longevity.
- Incorporate movement throughout the day: stretch, walk, or do mini-exercises.
5. Sleep & Recovery
- Keep a consistent sleep schedule.
- Wind down with a relaxing bedtime routine (reading, bath, gentle yoga).
- Avoid caffeine 4–6 hours before bed and alcohol 3–4 hours before bed.
- Reduce screens and bright lights 1–2 hours before sleep.
- Get morning sunlight and regular daytime movement.
- Consider natural aids: chamomile tea, magnesium, or melatonin (as advised).
- Discuss HRT with your doctor if sleep remains disrupted.
6. Mood & Stress Management
- Recognize hormonal impact on stress and mood: low estrogen → higher cortisol.
- Identify stressors: psychological, physical, and environmental.
- Reduce controllable stress: delegate tasks, set boundaries, simplify commitments.
- Regulate your nervous system: mindfulness, meditation, yoga, journaling, time in nature.
- Support your body: eat balanced meals, manage blood sugar, stay hydrated.
- Practice self-compassion and prioritize “refill” time for yourself.
7. Lifestyle Choices
- Alcohol: Minimize or stay under 10 units/week.
- Caffeine: Moderate or switch to decaf if it worsens symptoms.
- Tobacco: Avoid completely; seek help to quit if needed.
8. Consider Professional Support
- Discuss HRT or other medical options with your practitioner if symptoms impact quality of life.
- Consider working with a nutritionist or personal trainer, or seeing a menopause clinician for personalized guidance (we offer 1:1 online menopause consultations NZ wide)
- Use educational resources to stay informed and empowered.
9. Mindset & Self-Care
- View menopause as a time of renewal and new beginnings (Japanese term: konenki).
- Set small, achievable goals—dietary, lifestyle, or exercise-related.
- Build a supportive network of friends, family, or online communities.
- Celebrate small wins and recognize your body’s efforts during this transition.
10. Track Your Progress
- Keep a journal of:
- Symptoms and triggers
- Exercise and movement routines
- Sleep quality
- Mood changes
- Nutrition habits
- Adjust lifestyle strategies gradually and celebrate improvements.
By following this plan, you can reduce symptoms, support long-term health, and thrive during perimenopause and menopause, rather than just surviving it.
Final Words
Navigating perimenopause and menopause can feel overwhelming, both physically and emotionally. Be gentle with yourself, build a supportive network, and prioritize self-love and self-care.
Change takes time—set small, achievable goals and go at your own pace. Lifestyle strategies are powerful, and body-identical HRT can also be a helpful tool if symptoms are impacting your quality of life. Discuss options with your practitioner—it’s okay to combine lifestyle and medication for the best results.
The Japanese word for menopause is konenki, which means renewal years or energy – we love this phrase, as it changes our perception of menopause from a time of loss or negativity, to a time of new beginnings!!!
If you found this guide helpful, share it with others and follow us on social media for more tips. For an in-depth resource on optimizing health in perimenopause, menopause, and beyond, check out our comprehensive e-book here!
Here’s to thriving in this next chapter of life—stronger, healthier, and empowered❤️
REFERENCES :
Safabakhsh M, Siassi F, Koohdani F, Qorbani M, Khosravi S, Abshirini M, Aslani Z, Khajehnasiri F, Sotoudeh G. Higher intakes of fruits and vegetables are related to fewer menopausal symptoms: a cross-sectional study. Menopause. 2020 May;27(5):593-604. doi: 10.1097/GME.0000000000001511. PMID: 32068682.
Shifren JL, Gass ML, NAMS Recommendations for Clinical Care of Midlife Women Working Group. The North American Menopause Society recommendations for clinical care of midlife women. Menopause. 2014;21(10):1038-62. [PMID:25225714]
Bolland MJ, Leung W, Tai V, et al. Calcium intake and risk of fracture: systematic review. BMJ . 2015;351-365.
Tai V, Leung W, Grey A, Reid IR, Bolland MJ. Calcium intake and bone mineral density: systematic review and meta-analysis. BMJ . 2015;351-365.
Pludowski P, Holick MF, Pilz S, et al. Vitamin D effects on musculoskeletal health, immunity, autoimmunity, cardiovascular disease, cancer, fertility, pregnancy, dementia and mortality-a review of recent evidence. Autoimmun Rev. 2013;12(10):976-89. [PMID:23542507]
Kim JK, Park SU. Current potential health benefits of sulforaphane. EXCLI J. 2016. 15:5. 571-577.
Ruan, X., Seeger, H., Wallwiener, D. et al.. The ratio of the estradiol metabolites 2-hydroxyestrone (2-OHE1) and 16α-hydroxyestrone (16-OHE1) may predict breast cancer risk in postmenopausal but not in premenopausal women: two case–control studies. Arch Gynecol Obstet. 2015. 291. 1141-1146.
Bahadoran Z, Tohidi M, Nazeri P, Mehran M, Azizi F, Mirmiran P.. Effect of broccoli sprouts on insulin resistance in type 2 diabetic patients: a randomized double-blind clinical trial.. Int J Food Sci Nutr. 2012. 63(7). 767-771.
Axelsson AS, Tubbs E, Mecham B, Chacko S, Nenonen HA, Tang Y, Fahey JW, Derry JM, Wollheim CB, Wierup N, Haymond MW, Friend SH, Mulder H, Rosengren AH. Sulforaphane reduces hepatic glucose production and improves glucose control in patients with type 2 diabetes. Science: Translational Medicine. 2017. 9.
Connolly EL, Sim M, Travica N, Marx W, Beasy G, Lynch GS, Bondonno CP, Lewis JR, Hodgson JM and Blekkenhorst LC (2021). Glucosinolates From Cruciferous Vegetables and Their Potential Role in Chronic Disease: Investigating the Preclinical and Clinical Evidence. Front. Pharmacol. 2021. 12. 767975.
Tortorella SM, Royce SG, Licciardi PV, Karagiannis TC. Dietary Sulforaphane in Cancer Chemoprevention: The Role of Epigenetic Regulation and HDAC Inhibition. Antioxid Redox Signal.. 2015. 22(16). 1382-1424.
Palliyaguru DL, Yang L, Chartoumpekis DV, et al. Sulforaphane Diminishes the Formation of Mammary Tumors in Rats Exposed to 17β-Estradiol. Nutrients. 2020. 12(8). 2282.
Mayra ST, Johnston CS, Sweazea KL. High-nitrate salad increased plasma nitrates/nitrites and brachial artery flow-mediated dilation in postmenopausal women: A pilot study. Nutr Res. 2019 May;65:99-104. doi: 10.1016/j.nutres.2019.02.001. Epub 2019 Feb 22. PMID: 30954341.
https://aacrjournals.org/cebp/article/9/8/773/179852/Brassica-Vegetable-Consumption-Shifts-Estrogen
Liu ZM, Ho SC, Xie YJ, et al. Whole plant foods intake is associated with fewer menopausal symptoms in Chinese postmenopausal women with prehypertension or untreated hypertension. Menopause. 2015;22(5):496-504. [PMID:25387345]
Beezhold B, Radnitz C, McGrath RE, et al. Vegans report less bothersome vasomotor and physical menopausal symptoms than omnivores. Maturitas. 2018;112:12-17. [PMID:29704911]
Kroenke CH, Caan BJ, Stefanick ML, et al. Effects of a dietary intervention and weight change on vasomotor symptoms in the Women’s Health Initiative. Menopause. 2012;19(9):980-8. [PMID:22781782]
Yim G, Ahn Y, Chang Y, et al. Prevalence and severity of menopause symptoms and associated factors across menopause status in Korean women. Menopause. 2015;22(10):1108-16. [PMID:25783469]
Murkies AL, Lombard C, Strauss BJ, et al. Dietary flour supplementation decreases post-menopausal hot flushes: effect of soy and wheat. Maturitas. 2008;61(1-2):27-33. [PMID:19434877]
Lewis JE, Nickell LA, Thompson LU, et al. A randomized controlled trial of the effect of dietary soy and flaxseed muffins on quality of life and hot flashes during menopause. Menopause. 2006;13(4):631-42. [PMID:16837885]
Lethaby A, Marjoribanks J, Kronenberg F, et al. Phytoestrogens for menopausal vasomotor symptoms. Cochrane Database Syst Rev. 2013. [PMID:24323914]
Franco OH, Chowdhury R, Troup J, et al. Use of Plant-Based Therapies and Menopausal Symptoms: A Systematic Review and Meta-analysis. JAMA. 2016;315(23):2554-63. [PMID:27327802]
Chen MN, Lin CC, Liu CF. Efficacy of phytoestrogens for menopausal symptoms: a meta-analysis and systematic review. Climacteric. 2015;18(2):260-9. [PMID:25263312]
Barnard ND, Kahleova H, Holtz DN, Del Aguila F, Neola M, Crosby LM, Holubkov R. The Women’s Study for the Alleviation of Vasomotor Symptoms (WAVS): a randomized, controlled trial of a plant-based diet and whole soybeans for postmenopausal women. Menopause. 2021 Jul 12. doi: 10.1097/GME.0000000000001812. Epub ahead of print. PMID: 34260478.
Messina M. Soy foods, isoflavones, and the health of postmenopausal women. Am J Clin Nutr. 2014 Jul;100 Suppl 1:423S-30S. doi: 10.3945/ajcn.113.071464. Epub 2014 Jun 4. PMID: 24898224.
Jull J, Stacey D, Beach S, Dumas A, Strychar I, Ufholz LA, Prince S, Abdulnour J, Prud’homme D. Lifestyle interventions targeting body weight changes during the menopause transition: a systematic review. J Obes. 2014; 824310.
Kapoor E, Collazo-Clavell ML, Faubion SS. Weight Gain in Women at Midlife: A Concise Review of the Pathophysiology and Strategies for Management. Mayo Clin Proc. 2017 Oct;92(10):1552-1558.
Lonnie M, Hooker E, Brunstrom JM, Corfe BM, Green MA, Watson AW, Williams EA, Stevenson EJ, Penson S, Johnstone AM. Protein for Life: Review of Optimal Protein Intake, Sustainable Dietary Sources and the Effect on Appetite in Ageing Adults. Nutrients. 2018 Mar 16;10(3):360. doi: 10.3390/nu10030360..
Simpson SJ, Raubenheimer D, Black KI, Conigrave AD. Weight gain during the menopause transition: Evidence for a mechanism dependent on protein leverage. BJOG. 2023 Jan;130(1):4-10.
Nie, X., Xie, R. & Tuo, B. (2018). Effects of Estrogen on the Gastrointestinal Tract. Dig Dis Sci 63, 583–596.
Siddiqui, R.; Makhlouf, Z.; Alharbi, A.M.; Alfahemi, H.; Khan, N.A. The Gut Microbiome and Female Health. Biology 2022, 11, 1683. https://doi.org/10.3390/biology11111683
Veira, A.,
Castelo, P. et al, (2017). Influence of oral and gut microbiota in the health of menopausal women. Front. Microbiol. 8: 1884
Baylis, D., Bartlett, D.B., Patel, H.P. et al. (2013). Understanding how we age: insights into inflammaging. Longev Healthspan 2, 8. https://doi.org/10.1186/2046-2395-2-8
Ferrucci L. & Fabbri, E. (2018). Inflammageing: chronic inflammation in ageing, cardiovascular disease, and frailty. Nat Rev Cardiol. 15(9):505-522. doi: 10.1038/s41569-018-0064-2. PMID: 30065258; PMCID: PMC6146930.
Franceschi, C. et al. (2018) Inflammaging: a new immune-metabolic viewpoint for age-related diseases. Nat. Rev Endocrinology, 14(10):576-590.
McCarthy M, Raval AP. The peri-menopause in a woman’s life: a systemic inflammatory phase that enables later neurodegenerative disease. J Neuroinflammation. 2020 Oct 23;17(1):317.
Neves J., & Sousa-Victor, P. (2020). Regulation of inflammation as an anti-aging intervention. FEBS J. 287(1):43-52. doi: 10.1111/febs.15061 31529582.
McCarthy, M., Raval, A.P. The peri-menopause in a woman’s life: a systemic inflammatory phase that enables later neurodegenerative disease. J Neuroinflammation 17, 317 (2020). https://doi.org/10.1186/s12974-020-01998-9
Aslani Z, Abshirini M, Heidari-Beni M, Siassi F, Qorbani M, Shivappa N, Hébert JR, Soleymani M, Sotoudeh G. Dietary inflammatory index and dietary energy density are associated with menopausal symptoms in postmenopausal women: a cross-sectional study. Menopause. 2020 May;27(5):568-578. doi: 10.1097/GME.0000000000001502. PMID: 32068687.
Davis, S., Castelo-Branco, C. et.al. (2012). Understanding weight gain at menopause. Climacteric, 15: 419–429.
Reinke H. & Asher G. (2017). Circadian clock control of liver metabolic functions. Gastroenterology, 150: 574–580.
North American Menopause Society (12th Oct. 2022). Hot flashes are not just uncomfortable but also could be hard on the heart
Kodoth V, Scaccia S, Aggarwal B. Adverse Changes in Body Composition During the Menopausal Transition and Relation to Cardiovascular Risk: A Contemporary Review. Womens Health Rep (New Rochelle). 2022 Jun 13;3(1):573-581.
Biglia N, Cagnacci A, Gambacciani M, et al. Vasomotor symptoms in menopause: a biomarker of cardiovascular disease risk and other chronic diseases? Climacteric. 2017;20(4):306-312. [PMID:28453310]
Franco OH, Muka T, Colpani V, et al. Vasomotor symptoms in women and cardiovascular risk markers: Systematic review and meta-analysis. Maturitas. 2015;81(3):353-61. [PMID:26022385]
Lee, E., Anselmo, M, Tahsin, T. et al. Vasomotor symptoms of menopause, autonomic dysfunction, and cardiovascular disease. 2022, Am. J. of Physiology
Stachowiak G, Pertyński T, Pertyńska-Marczewska M. Metabolic disorders in menopause. Prz Menopauzalny. 2015 Mar;14(1):59-64. doi: 10.5114/pm.2015.50000. Epub 2015 Mar 25.
Daley A, Stokes-Lampard H, Thomas A, et al. Exercise for vasomotor menopausal symptoms. Cochrane Database Syst Rev. 2014. [PMID:25431132]
Daley A, Macarthur C, Stokes-Lampard H, et al. Exercise participation, body mass index, and health-related quality of life in women of menopausal age. Br J Gen Pract. 2007;57(535):130-5. [PMID:17266830]
Ayers B, Smith M, Hellier J, et al. Effectiveness of group and self-help cognitive behavior therapy in reducing problematic menopausal hot flushes and night sweats (MENOS 2): a randomized controlled trial. Menopause. 2012;19(7):749-59. [PMID:22336748]
Daley A, Stokes-Lampard H, Macarthur C. Exercise for vasomotor menopausal symptoms. Cochrane Database Syst Rev 2011 5:CD006108.
Carpenter JS, Burns DS, Wu J, Otte JL, Schneider B, Ryker K, Tallman E, Yu M. Paced respiration for vasomotor and other menopausal symptoms: a randomised controlled trial. J Gen Intern Med 2013 28:193–200.
Woods, N. et al. (2009). Cortisol Levels during the Menopausal Transition and Early Postmenopause: Observations from the Seattle Midlife Women’s Health Study. Menopause, 16(4): 708–718
Saensak S, Vutyavanich T, Somboonporn W, et al. Relaxation for perimenopausal and postmenopausal symptoms. Cochrane Database Syst Rev. 2014. [PMID:25039019]



